Workplace Reopening Guide
Guidelines for Reopening Safely
Eventually we will reach the other side of the COVID-19 pandemic. However, that “other side” will be months if not years away. Meanwhile, Arizona and many other states are looking for guidance on how to “reopen” in a way that is safe for our communities, and at the same time provides enough flexibility so we can all get back to work and back to school.
Remember, based on what we know now, up to 40% of people infected with COVID-19 may not feel sick or have any apparent symptoms. When people are infected but not sick, that is what health experts call “asymptomatic” (they have no symptoms). So even people who don’t feel sick could be infected and spread the virus. That is why these workplace guidelines are so important.
Science Based, Expert Guided
This Workplace Reopening Guide resource webpage is based on the best current science related to COVID-19. The guide also draws upon the infection prevention guidelines that have been developed by experts based on years of scientific research conducted during previous outbreaks, both viral and bacterial.
All of the guidance included here comes from faculty and researchers at the Mel and Enid Zuckerman College of Public Health (MEZCOPH) at the University of Arizona. The information builds on the knowledge and expertise that those faculty have developed in the fields of epidemiology and infection prevention. It is important to remember that the “3 Ts” – Testing, Tracing, and Treating – must be at the center of any effort to resume social and business activities in our region, our state, and our nation. The guidelines presented here are designed to support the “3 Ts” approach.
All of the information included in the Guide is intended to supplement the recommendations provided by the State of Arizona, the Arizona Department of Health Services, Pima County Health Department, and the US Centers for Disease Control (CDC). Additional guidance can be found on the websites for those organizations, all the names are hotlinked.
The Pyramid of Prevention Sets Priorities for Infection Prevention in the Workplace
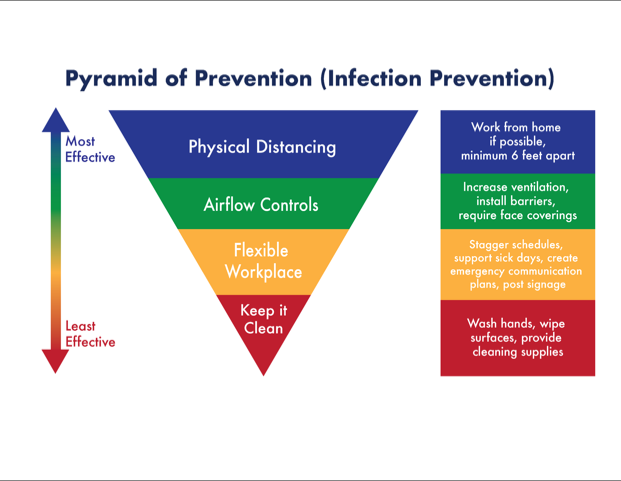
The Pyramid of Prevention was created by Kelly Reynolds and researchers in the Environment, Exposure Science and Risk Assessment Center (ESRAC) at the University of Arizona. Graphic by Rachel Larson, MEZCOPH public health student.
Yes, the Pyramid is upside down. This “Pyramid of Prevention” graphic shows the best measures that can be used in the workplace to stop the spread of COVID-19, starting with the most effective measures at the top. The inverted pyramid shape is especially useful to visualize the best practices for “reopening” the workplace because it shows what measures are most effective and should be the highest priority.
The priority levels in the Pyramid go from Physical Distancing at the top (the most important precaution), descending down through levels of priority to Keep It Clean. All the prevention measures are important, but some of them are much more important because they are much more effective.
Make Space in the Place
[Physical Distancing]
As you can see, the most effective way to stop the spread of COVID-19 in the workplace is by maintaining distance between people. If you and your employees are in the same building, keep everyone at least 6 feet apart. The virus spreads through microscopic droplets in the air, what health researchers call “aerosols,” and they very rarely travel more than 3-6 feet. If we keep our physical distance (we all need some space!), the virus will have a hard time spreading. The layout of the workplace can make a big difference by keeping people spaced apart.
Get More Air in There
[Airflow Controls]
The second priority is Airflow Controls. What does that mean? The three big things we can “engineer” in the workplace to prevent the spread of COVID-19 are: ventilation, barriers, and face masks.
Ventilation is vital. We want to get as much fresh air into the workplace as we can to dilute any virus that might be in the air. That is why the virus has a harder time spreading outdoors, because the air moves, the breeze blows, and any tiny viral droplets are quickly dispersed.
Barriers are effective. Many of us have seen the Plexiglas barriers at the grocery store checkout. They really work! The barriers stop the microscopic droplets called “aerosols” from traveling.
Face masks also serve as a barrier and they help significantly to prevent the spread of COVID-19. If someone is sick and does not know it (the person is asymptomatic), and that sick person is wearing a face mask , the face mask will help prevent the release of viral droplets into the air, droplets the sick person can discharge when talking or even breathing.
Good ventilation for the workplace, along with barriers and face masks for people, are important prevention measures to stop the spread of COVID-19.
Stagger Schedules and Make Sure Sick Workers Stay Home
[Flexible Workplace]
At the third level of infection prevention we focus on Administrative Controls. Those are the decisions about who works, when they work, and safety protocols to follow that the person in charge can make. When possible, the Administrator can stagger work schedules so that fewer employees are in the same space at the same time.
Administrators can also strategically change where people work or where they sit to keep them further apart and support the top priority (Physical Distance). They can also make sure that anyone who is sick must stay home and has the financial support they need to stay home. Workers need to be able to buy food and pay the rent. At the same time, if they come to work sick, they risk infecting others in the workplace, at a far greater economic toll.
Depending on the workplace, daily temperature checks for all employees when they arrive at work can be an effective health assessment. To maintain privacy and safety, administrators may want to utilize a barrier or partition and ensure the person taking employees’ temperatures is wearing appropriate protective gear.
And finally, Administrators can effectively communicate to their employees about how to prevent the spread of the virus, provide training materials, and have emergency communication plans in place.
Wash Your Hands, Wipe the Surfaces
[Keep It Clean]
At the bottom of the inverted Pyramid of Prevention is the Keep It Clean layer. A clean workplace is important. When you reopen a workplace, review and implement new cleaning and hygiene practices. Everyone should wash their hands frequently. Administrators can place alcohol-based hand sanitizing stations in high trafficked workplace areas – make sure the stations are re-filled regularly! Provide tissues, no-touch trash cans, and disposable towels to encourage good hygiene. Routinely clean high touch surfaces such as door knobs, phones, light switches, and keyboards with disinfectant. These practices will help stop the spread and protect employees’ health and wellness.
If an employee gets sick, close off all affected areas used by the employee, open all windows and doors, and wait 24 hours before cleaning and disinfecting.
CDC Guidelines for Cleaning and Disinfecting Workplaces if an employee gets sick can be found at https://www.cdc.gov/coronavirus/2019-ncov
Prevention Measures Infographic Guides for Workplaces
The Pyramid of Prevention above provides an overall context for prevention measure priorities for the workplace. All the infection prevention graphics included below can also be very helpful to educate workers, and they all apply within the larger Pyramid of Prevention framework. These graphics were created based on research and best practices developed by the faculty at the Zuckerman College of Public Health at the University of Arizona. Most of the infographics offered here were created by public health student interns in the Academic Health Department at MEZCOPH under the guidance of Emily Waldron.
We will continue to add infographics and videos to the Workplace Reopening Guide as they become available.



